Gastrointestinal Disorders: Causes, Symptoms And How To Achieve A Healthier System
Last updated on
Unfortunately, among the most common problems with the population today are gastrointestinal disorders, with the most common symptoms such as constipation and diarrhea.
People are consuming less nutritious foods, are over-stimulated and stressed, are not maintaining healthy exercise habits and are damaging their entire bodies with highly processed, chemical-laden food from man rather than from Nature.
Understanding if you have chronic constipation and addressing the concern with your doctor (and nutritionist), can save you from suffering from a condition or allowing a disease to progress. Individuals over 50 years of age are at increased risk of Crohn’s disease, bowel polyps and ulcerative colitis, and are recommended for medical screening (1).
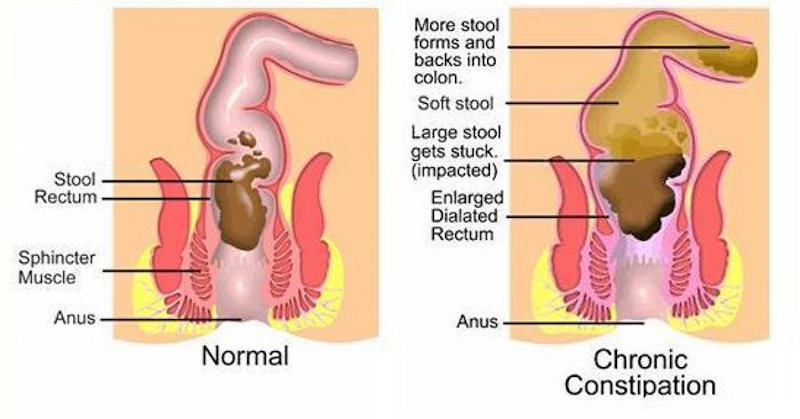
Chronic Constipation
Chronic constipation is a common condition that is characterized by dry and tightly packed fecal matter in the colon that lead to difficult, infrequent and incomplete bowel movements. The sufferer would experience difficulty in eliminating very little, dry, and hard stools. Bowel movements are usually strenuous, and there is a constant feeling of fullness or bloating.
Stress Can Increase Constipation
One of the main triggers of constipation in today’s fast paced world is stress. The gut is also known as the “second brain” because of its interaction with the brain. The gut influences the same neurotransmitters affected by emotions such as anger and anxiety and has more neurons lining the gut than are contained in the spinal cord (9, 10).
Next time you can’t control your emotions, ask yourself if the stress is worth an ulcer or not.
Stress Creates That “Gut Feeling”
Have you ever been cautious about a certain scenario and you communicated to someone that you “had a gut feeling”?
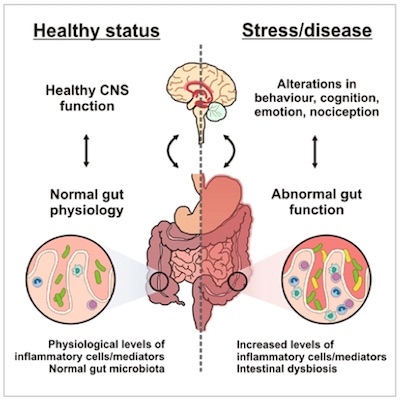
Think of a time that you may have been frightened; perhaps at night while sleeping alone somewhere new and you hear a suspicious sound outside your door. Was the first thought that came to mind, I need to poop? Of course not!
Your body responded with an increased heart rate, dilated pupils and a heightened sense of preparing your body for a fight or flight.
With prolonged stress, your body signals to your body to hold all bowel movements, eventually resulting in chronic constipation.
Medications Can Cause Constipation
If chemicals naturally secreted by the body to defend against stress affect the frequency in which you are able to poop, it should be obvious that medications should have the same consequences. Medicines that are known to cause constipation include antihistamine drugs, antidepressants, chemotherapy drugs and analgesic drugs such as opioids.
These drugs have been found to be the cause of constipation in 90% of cancer patients and up to 40% of non-cancer patients (2).
Conditions Associated With Constipation
Problematic symptoms associated with the formation and movement of stool throughout your body may manifest in a variety of symptoms. Irrelevant of color, the symptom of constipation alone is linked to a variety of conditions and diseases.
1. Colorectal Cancer
Although constipation may simply result from dehydration and other reasons stated above, if you have a history of colon cancer or inflammatory bowel disease (IBD) in your family, you should get tested.
2. Ulcerative Colitis
Ulcerative colitis (UC) is a disease that is strongly associated with the increase in white blood cells in the colon (2, 4). These cells produce inflammation in order to defend the body from infection and trigger a domino effect of health consequences.
Inflammation increases the permeability of the intestine and allows harmful bacteria to sneak through gaps and cause infection in neighboring organs.
3. Constipation-Dominant IBS
Irritable bowel syndrome (IBS) is the most frequently diagnosed gastrointestinal disorder affecting an estimated 90 million people worldwide (6). IBS results from a change in the movement of gas through the intestines leading to abdominal pain, constipation or diarrhea. Researchers are learning that these patients have a problem with their guts, possibly a result of the mind-gut connection. (4)
Scientists have noticed a significant difference in how the brain responds to anxiety and fear in individuals with IBS. The link between the brain and the gut is, therefore, partially responsible for the secretion, absorption and motility of stools through the intestines.
Another cause of IBS may be a result of decreased healthy bacteria such aslactobacilli and bifidobacteria. These two kinds of bacteria compete with pathogens to take up space and do not stimulate gas production. Studies have found that IBS patients have decreased activity of these bacteria in the colon. (4)
IBS is also related to small intestinal bacterial overgrowth (SIBO). This is where there is an overgrowth of bacteria in the small intestine. SIBO damages the intestinal lining and creates a state of mild-to-severe leaky gut syndrome, resulting in food allergies, sensitivities and chronic inflammatory processes (2). The malnutrition and inflammation this causes can lead to bouts of diarrhea and constipation.
4. Psychological Stressors
Constipation is frequently problematic in people suffering from depression, anxiety, and eating disorders. Again, the mind is so intrinsically designed and effective at prioritizing life’s demands that at times it might seem like it can work against us.
5. Neurological Problems
Especially in people over 50 years of age, constipation can be a cause for concern because of the effects that nerves play in connection to the gut. A long-term change in your bowel habits may be an indication of dementia, muscular dystrophy, stroke or Parkinson’s disease (2).
Conditions Associated With Chronic Diarrhea
Although constipation may seem like a more dominant problem, diarrhea can also be a sign of declining health. Despite the frequency of bowel movements, diarrhea is associated with 3 of the 7 types of poop according to the Bristol Stool Scale. Individuals suffering from diarrhea typically have an infection due to bacterial overgrowth (7).
1. Infection
The microbiota, or gut environment, needs to be a priority for maintaining a healthy bowel regimen. The colon can contain upwards of 500 to 1,000 different bacterial species influenced by diet, environment, age and antibiotics. An overgrowth of bad bacteria and viruses can lead to a gut infection and resulting in diarrhea.
Healthy bacteria in the gut can relieve symptoms associated with diarrhea and prevent the body from infectious agents such as harmful bacteria (6, 11).
2. Bile Acid Malabsorption
Researchers recognize that diarrhea may be an under-appreciated symptom of bile acid malabsorption. Bile acid is produced by the liver to help absorb lipids in the small intestine. Diarrhea can, therefore, be a signal from your body that a greater problem exists.
Disorders may include Crohn’s disease, Celiac disease (gluten intolerance), liver cancer or pancreatitis. (5, 6)
3. Diarrhea-Dominant IBS
Diarrhea is also associated with IBS symptoms. If diarrhea is a persistent problem, IBS may be to blame (3). Weight loss might be another side effect that results in individuals who have diarrhea-dominant IBS.
4. Diabetic Diarrhea
Gastrointestinal disorders are common among those affected by long-standing history of diabetes. Left unmanaged, chances are that they will develop a peptic ulcer, gallstones, IBS, reflux, constipation, abdominal pain, nausea, vomiting, and frequent diarrhea.
Chronic diarrhea in diabetics may be related to problems in the small bowel or colon. Abnormally rapid transit of fluids may occur in the colon, leading to increased stool frequency and urgency. In addition, abnormalities in the absorption and secretion of colonic fluid may develop, leading to increased stool volume, frequency, and water content.
Many patients go undiagnosed and under-treated because the GI tract has not been traditionally associated with diabetes and its complications.
16 Ways To Achieve Healthy Bowel Movements
You may snicker at the concept that there is actually a way to maintain regularity and achieve a healthy poop, but it is essential not only to promoting a healthy gastrointestinal tract but also to achieving optimal health and vitality. If increased energy and happiness is what you desire, set all awkwardness aside and prioritize your goal to achieve healthier bowel movements.
In time you may learn how to develop a healthy stress management response by removing stressors in your life or by calming your mind through the practice of breathing techniques. In the meantime, the following tips can help you achieve success by making a few changes in your lifestyle now.
1. Cop A Squat
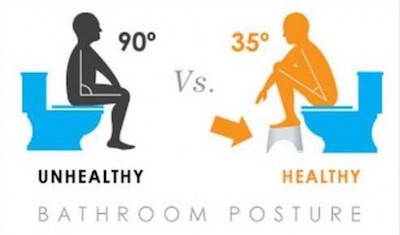
After all, our ancient ancestors likely found themselves digging holes and squatting to poop and you should be doing the same.
Placing your feet on a stool or trash can and leaning forward relieves the tension from your intestines and allows you to eliminate waste with greater ease.
2. Hydration

Or perhaps you are excessively consuming caffeinated or sugary beverages that further deplete nutrients in the body that aid bowel movements.
Increase your daily consumption of water and fresh juices; decrease drinks that may be adversely affecting your health.
In the summertime, I recommend drinking three quarters of your body weight in ounces of water. Drink 8-24oz of clean water first thing in the morning (and give yourself 30 minutes to an hour before eating) to help induce gut motility and healthy bowel activity. The morning is the most active time for your colon and the best time to eliminate waste.
3. Salt Water
The salt-water flush has been used for centuries to improve bowel motility. Simply take 1 teaspoon of seasalt in 2-4 oz of water and swallow it. Follow this up with 8-16oz of water. The salt helps to flush the colon so be sure you have some time over the next 1-2 hours to spend in the bathroom.
4. Avoid Processed Foods And Alcohol
Having to wipe too many times may be a consequence of excessive mucus in your colon. Eliminate or reduce manufactured and highly processed foods and alcohol from your diet. I would also advise to stay away from gluten, pasteurized dairy, soy, corn and peanuts.
5. Medication Intervention
Medications affect gut health and produce common side effects such as constipation and diarrhea. Have a conversation with your prescribing physician and discuss if pharmaceutical drugs are causing you more harm than good.
6. Increase Healthy Gut Bacteria

Introduce healthy bacteria into your diet by taking a daily probiotic and consuming fermented foods such as sauerkraut, kimchi, coconut yogurt and coconut water kefir.
Probiotics increase intestinal health and protect against inflammation, increased permeability apparent in those with leaky gut syndrome and hypersensitivity concerns in patients with IBS and psychological disturbances (4).
7. Avoid Food Allergens And Sensitivities
You may already be aware if specific foods such as processed foods, wheat, dairy or cured meat products increase abdominal discomfort and change the frequency or urge to poop (4). Test for and avoid food sensitivities using a biofeedback test or specific blood test.
8. Increase Fiber
Fiber can be found in a supplement source typically containing psyllium but it is best to receive the benefits of fiber from Nature. Increase the amount and variety of fruits and vegetables into your diet. Individuals consuming plant-based diets have been studied to have fewer carcinogens in their microbiome than those who primarily consume meat (5, 2).
9. Reduce Reliance On Laxatives
Although traditional laxatives may be the first offensive move to treat constipation, laxatives have not significantly proven beneficial at relieving pain and may aggravate the problem. Instead of relying on a laxative in pill form, try a more natural approach by drinking apple, pear or prune juice (2, 4).
10. Don’t Hold It In
You may be taken back by the necessity to poop in a public bathroom, but when you need to go you should go. Holding it in allows water and nutrients to be reabsorbed back into the body. Poop is waste. When the urge presents itself, do not hesitate to go.
11. Supplement Magnesium Into Your Diet
Magnesium can stimulate the movement of stool through the bowels by serving as a muscle relaxant (8). Magnesium is easily depleted under chronic stress but can be replenished in our food supply. Excellent food sources of magnesium include green leafy vegetables, nuts, seeds and some fruits such a bananas and apples.
The best form of magnesium for improving bowel activity is magnesium oxide which is found in our Daily Detox supplement which I often use with clients that have digestive complaints.
12. Exercise
Increasing physical activity has provided significant health benefits both physically and emotionally. Inducing a cardio-respiratory fitness response increases oxygen consumption in the body.
Exercise has been studied to decrease the frequency of pain, regulate bowel movements, combat fatigue, decrease cortisol and alleviate symptoms of depression and anxiety (3).
13. Proper Testing for SIBO Or Candida
Unhealthy stools are a red flag sign of microbial dysbiosis. This is often due to small intestinal bacterial overgrowth (SIBO) or Candida. Read up on these health problems and get the proper testing, diagnosis and treatment to heal your gut.
14. Carminative Herbs

They also tone the mucous surfaces and increase peristaltic action within the esophagus to the stomach. This peristaltic action propels food and wastes through the system.
The major carminative herbs include cilantro, cinnamon, ginger, juniper, anise, fennel, cloves, caraway, dill, peppermint, thyme and licorice.
These carminatives are often combined with aloe vera. Aloe vera is a cathartic herb that increases intestinal transit time and is used to alleviate constipation. This combination helps stimulate effective and comfortable stools for those with chronic constipation.
15. Smooth Move Tea
Used for thousands of years to get your bowel moving again, senna works by gently stimulating your intestines and aiding your body’s natural elimination process.
This tea combines senna with the carminative herbs fennel, cilantro and ginger to reduce the potential for unpleasant feelings like cramping. Smooth Move tea is best taken at bedtime to help improve bowel movements the following morning. However, this is still a form of laxative and is not recommended as a long-term solution.
16. Gut Repair Supplement
This supplement combines aloe vera along with the carminative support of deglycyrrhizinated licorice extract. It also contains L-glutamine which helps to form good healthy stools and a powerful prebiotic fiber in arbinogalactan.
Arbinoglactan minimizes ammonia synthesis and absorption, enhances production of short chain fatty acids and increases the gut microflora population. It is one of the best fiber sources for healthy bowel movements. I use this supplement for clients with leaky gut syndrome, irritable bowel syndrome, diarrhea and constipation issues.
This article is shared with permission from our friends at drjockers.com.
Some of the links I post on this site are affiliate links. If you go through them to make a purchase, I will earn a small commission (at no additional cost to you). However, note that I’m recommending these products because of their quality and that I have good experience using them, not because of the commission to be made.
































 JOIN OVER
JOIN OVER
Comments