Mammography Vs Thermography For Breast Cancer Screening And Early Detection
Last updated on
Are you looking for information on breast cancer screening? Well, it is absolutely a smart idea to have a regular examination for early detection, especially if you have a positive family history for the same (in this case, screening is recommended from an earlier age). However, the method of screening that you choose must be safe.
Breast cancer is not an unusual disease. A study meta-analysis concluded for the year 2012, the following statistics:
- New cases of breast cancer diagnosed in 2012 reached up to a figure of 1,617,149
- The mortality rate for the same scored 521,907
With the growing advancements in medical technology, several modalities are now accessible that can help in detecting the presence of breast cancer cells at various stages.
Conventional Breast Cancer Screening Methods
It is always good to know about the basics and types of the available approaches for early cancer detection. You can discuss with your healthcare provider regarding the method you should use. The conventional breast cancer screening methods are:
- Physical examination: This method is suggested by doctors to women of all age groups. Manually palpating your breasts and armpits deeply in a clockwise manner will reveal any underlying lump or abnormal mass. You can do this once a month several days after your period ends. In case you suspect the presence of any lump that wasn’t there before, get it checked by your doctor.
- Ultrasound: Using ultrasonic waves, the anatomical contour of breast tissue and blood vessels can be traced and lesions can, therefore, be detected. In case your doctor confirms a lump in your breasts or axilla on clinical examination, the next step that they most probably will advise may be an ultrasound to confirm the presence.
- Mammography: A mammogram is employed to look into the detailed structure of breast tissues. The healthcare system generally recommends mammography for women of older age groups as breast density remains a limiting factor here.
- Biopsy: This is rather an invasive modality of diagnosis and it brings about the most definitive results. In cases of high suspicion, a doctor will have to advise for fine needle aspiration and biopsy.
Just How Safe Is Mammography?
At present, mammography is one of the most-widely used methods for screening breast cancer.
A study published in The Lancet Oncology in 2011 demonstrated for the first time, that women who received the most mammography breast screenings had a higher cumulative incidence of invasive breast cancer over the following six years than the control group who received far less screenings.
Dr Veronique Desaulniers, founder of BreastCancerConqueror.com, is a Doctor of Chiropractic who herself had been a victim of breast cancer. She now helps women from all around the world to live their best life through healing of their body, mind and soul.
Dr V (as she is famously known) has this to say in the video above:
“Well, let’s start with mammograms. Again, by the time they see a lump on a mammogram, it has taken five to eight years to develop. And if a woman follows the 10-year protocol of getting a mammogram every year or every six months, she is getting as much radiation as a woman had at Hiroshima; the atomic bomb, if she stood a mile away from the epicenter. She is getting over 5 rads of radiation in a mammogram if she follows the traditional methods of mammography.
So mammograms cause a lot of problems – the compression, the radiation. Studies have shown that they can increase your risk of cancer. And the new study that came out in Canada, it was a 25-year study where they found that mammograms did not decrease breast mortality rate at all. In fact, they were just as effective as a self breast exam that women do.
So if we put mammograms aside and we look at the technology with thermography, which has been around for years and can detect physiological changes at a very early stage, wouldn’t you rather know that there is possibly some changes going on in your breast or in your abdomen five to eight years before you have a diagnosis? And with thermography, there is no pain, there is no compression, there is no radiation. It is just a beautiful tool to have in your pocket.”
Source: thetrutchaboutcancer.com
Thermography For Breast Cancer Screening – Accurate And Early Diagnosis
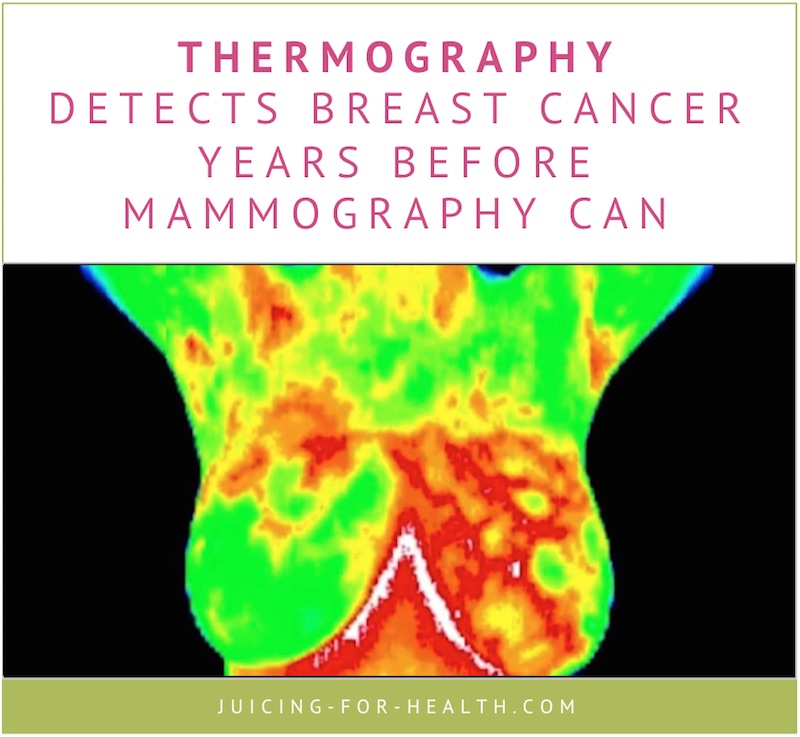
Thermography, also known as Digital Infrared Thermal Imaging (DITI), is employed to mark the heat areas of your body by the virtue of its ultra-sensitive, high-resolution digital infrared rays (IR) cameras.
Breast cancer involves inflammatory processes and the mediators of this course release heat. Using thermographic techniques, the scanner is able to create a temperature map of your body that can illustrate the greater heat-producing areas clearly. This is how your doctor may be able to trace the abnormal cellular processes and by the help of which, further diagnostic procedures and course of the disease can be evaluated.
How Does Thermography Work To Detect Early Cancer?
Every cell in our body naturally gives off some small amount of metabolic heat that increases in temperature when an abnormal condition occurs. A thermographic camera is able to detect these natural heat that the body emits at a cellular level. It makes thermal imaging possible in that it’s able to detect abnormal activities five to eight years before a lump can be detected by mammography.
In their earliest stages, multiplying cancer cells are highly metabolic and need an abundant supply of nutrients to maintain or accelerate their growth. In order to grow, they increase circulation to their mutilated cells by keeping blood vessels open, activate inactive blood vessels, and create new ones (a process known as neoangiogenesis).
These vascular processes cause an increase in temperature in the affected regions. Whereas the newly formed and the activated blood vessels have a distinct appearance that thermography can detect even at that early stage.
Of course, in the presence of precancerous and cancerous cells and with all that multiplying activities going on, inflammation is definite. Inflammation emits heat that shows up in a thermogram. This is why thermography is often used to detect not only inflammation and cancer growth, but also other changes in the human body such as infections, trauma, allergies, flu or fever.
Thermography Over Mammography For Breast Cancer Screening
If cancer is caught in it’s early stage, there is a better chance of treating it successfully. And, because at at early stage, it has less likely to spread, a simple surgery may be able to remove them.
Latest research works have been successful in favoring thermography for breast cancer screening for early detection. Here is how it is emerging as a promising technique for the upcoming years:
Tracing heat patterns of the breast cells can predict the course of the disease as well as the risks quite earlier than its outcome. A study was conducted that involved 1,245 women who underwent:
- physical examination
- ultrasonic investigation
- mammography
- fine needle aspiration
- biopsy for breasts
One-third of the subjects showed up with histologically-proven cancers within a time frame of five years. In their cases, thermography was able to detect metabolic changes in the lesion cells that had the potential to grow rapidly, and its predictive value remains far better than that of a biopsy.
When opting for a procedure, you would certainly want to decide in favor of the one that yields accuracy of high scores. Experimental studies have been successful in concluding that cell patterns exhibited on a thermogram are nearly 80 percent accurate. Hence, thermography takes an edge over mammography.
With mammogram, it may be harder to peak through the anatomical abnormalities of denser breast tissues, especially those of premenopausal women.
On the other hand, in a study that compared efficacies of the three most-adopted breast cancer screening modalities: clinical examination, mammography, and thermography; the certainty of the thermography for larger lesions and for the ones with lymph node metastasis was significantly lower as compared to that of mammography.
A compelling reason that questions the role of mammography is the high probability of “false positive results”. A retrospective cohort evaluation for breast cancer screening and diagnosis of 2,400 women subjects falling between the ages of 40 and 69 years led to the discovery that, mammography stood for a cumulative risk of 49.1 percent of false positive results on an estimate. The research included four mammograms and five clinical breast examinations per subject over a 10-year period.
5 Advantages of Opting For Breast Thermography Screening
1. Suitable for younger women
It should be the first choice for premenopausal women whose breasts tend to be denser. Thermography can differentiate fibrocystic tissue, scars or breast implants from that of cancerous cells.
2. Detect cell changes outside of the breast region
Many times precancerous cells can start forming from the armpit area due to use of underarm deodorants, and the concentration of lymph nodes in that area. Mammography is not the best method to use for screening outside of the breast region, the armpit area included.
3. Great as an additional test
Whatever method you decide to use, thermography will be a great additional test due to its accuracy and early detection ability. Should you discover a lump from your self-examination, a thermography will be able to give you a more conclusive diagnosis as to the type of lump/growth it is.
4. It is painless and radiation-free
As you may have experienced or heard from other women, the pressure of a mammogram machine is equivalent to putting a 50-pound weight to compress your breasts. Many who have done mammogram will be able to tell you that it is painful. And this is especially traumatic for women who have small breasts.
It doesn’t make sense to use high exposure to radiation from mammography to find what we know is caused by radiation!
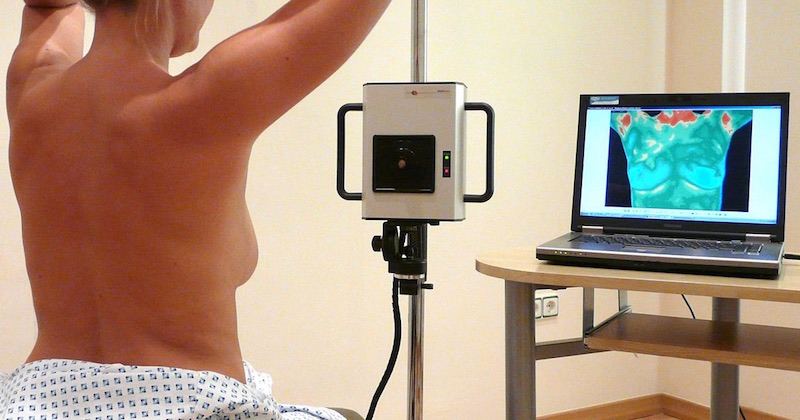
With thermography, you will be required to sit in front of the scanner that scans your body heat. Thermography is non-contact, non-invasive, uses no painful breast compression, nor emits any harmful radiation.
5. It is safe
Thermography is so safe that it can be used on pregnant and nursing women without any side effects whatsoever. It’s merely taking an image of your body heat, like shooting a photo!
Is Thermography Available In Your Country?
Since posting this article, I’ve received many emails from readers asking if thermography is available in their countries. So, here’s my answer:
The only way to find out if thermography is available in your country is to google it. Use the keywords “thermography”, “thermal imaging” or “thermography breast screening” and your country.
In some countries, you may come across sites that say that “Thermal Imaging is not approved …”, or “…. not encouraged”, or similar phrases. These are often countries where conventional methods such as mammography dominates. Despite these statements, chances are high that your local alternative medicine clinics may offer these services.
In which case, google “thermal imaging” or “thermography screening” and your city name, to find an alternative medicine clinic that provides such a service. In bigger cities, you would most likely find this service available. All the best!
Conclusion About Thermography
As with anything so important as your health, I suggest that you make an informed decision. Know the source of your information. There will always be two sides to healthcare. There is the conventional, invasive method; and there is the traditional, holistic and natural approach. Decide which route you wish to take.
You may have been told or formerly educated about mammogram but now decided that it is, after all, not the best way to go. There is no need to feel any guilt nor be intimidated into going that route. Take your own health into your own hands and decide what you think is best and safe.
When done properly, thermography for breast cancer screening has the true potential to detect breast cell anomalies long before mammography can detect cancer. By early detection (up to eight years earlier), it allows you to get help and implement lifestyle changes that can improve your health significantly.
References:
- Ghoncheh M, Pournamdar Z, Salehiniya H. Incidence and Mortality and Epidemiology of Breast Cancer in the World. Asian Pacific journal of cancer prevention : APJCP. 2016;17(S3):43-6. web-link
- Gautherie M, Gros CM. Breast thermography and cancer risk prediction. Cancer. 1980;45(1):51-6. web-link
- Schaefer G, Závišek, M. and Nakashima, T. . Thermography based breast cancer analysis using statistical features and fuzzy classification. Pattern Recognition. 2009;42(6):1133-7. web-link
- Feig SA, Shaber GS, Schwartz GF, Patchefsky A, Libshitz HI, Edeiken J, et al. Thermography, mammography, and clinical examination in breast cancer screening. Review of 16,000 studies. Radiology. 1977;122(1):123-7. web-link
- Elmore JG, Barton MB, Moceri VM, Polk S, Arena PJ, Fletcher SW. Ten-year risk of false positive screening mammograms and clinical breast examinations. The New England journal of medicine. 1998;338(16):1089-96. web-link
Some of the links I post on this site are affiliate links. If you go through them to make a purchase, I will earn a small commission (at no additional cost to you). However, note that I’m recommending these products because of their quality and that I have good experience using them, not because of the commission to be made.
Comments
Leave a Reply





























 JOIN OVER
JOIN OVER
Hi Sara, Interesting article. Do you know of any countries that participate in thermography?
Hi Luisa, thermography scanning for breasts has been used by many countries as far back as more than a decade ago. It is being used extensively in advanced countries such as Japan, Korea, China and Germany. Unfortunately, the use of thermography is discouraged in North America, in favor of mammography that emits a high dose of radiation. However, you may still be able to find alternative medicine practitioners in North America who offer this service.
Could you publish the cities and states in the USA?
I’ll definitely be asking my doctor about this before my next screening. Thanks for posting this. (BTW, it’s “If cancer is caught in its early stage. . .” not “it’s early stage”.)
Is this available in my area,? I live in kitty hawk nc closest big city is Norfolk Va
Is it suitable for myself if I’ve already been treated for breast cancer? I’m 60 yrs old
So… IF thermography finds an area of suspicion, what happens next. No surgeon will biopsy or excise on thermography alone. There will be a mammogram, and ultrasound and then a biopsy. Thermography alone DOES NOT DIAGNOSE CANCER.
How do I find a doctor or clinic that does thermography in the. Dallas area?
This article has an incredible amount of misinformation.
Hello
I should like to pint out that Dr V is completely wrong to compare 10 years of mammograms to 1 mile from the epicentre of Hiroshima. The amount of radiation is way off.
I think it’s irresponsible to scare people away from life saving tests in this way. The dose for a mammogram is 0.4 mSv this adds up to 8mSv if a woman attends for a mammogram every 6 months for 10 years.
The dose 1 mile away from the epicentre of Hiroshima was 360mSv.
She should check her facts before spouting such nonsense.
If you are getting your information on breast cancer from a juicing website you are definitely doing it wrong.
Thanks to an INCOMPETENT tech in Boardman Ohio the ruptured both of my implants.I have been through hell since 1980. I have had 5 breast surgery due to her compressing my breast so hard my left implant ended up in my left armpit and tricep.
What is the cost of this test please or is it covered by ohip?
is this only for breast cancer and why skin cancer facial? , and who makes the cameras
I have a lump they are watching
What information do you have about mammary contact thermomamography? What thermomamography equipment would be indicated for breast screening. Thank you
Are you close to LA? How we get ur advice and visit you?
How can I get information on this new test
Am interested in this procedure in Fresno, Ca. Please advise where I can have this done!
I would take this down because the facts are wrong. I do mammography. The fact that u get as much radiation as 1000 chest xrays is totally wrong! Misleading the public is so unfair and wrong and u are possibly letting women not get properly checked which could lead to their death! I cannot believe anyone promoting health and wellness would post anything that has not been verified properly. I am big about healthy alternatives to many things but to lie to scare women is not the thing to do. PLEASE FACT CHECK before putting people’s lives at risk!
You need to be properly educated in radiography. A mammogram is nowhere near as much radiation as 1,000 chest X-rays, that is harmful misinformation and can cause a delay in early detection for breast cancer by telling women not to get their mammograms done. Shame on you for making such a bold, untrue, hyperbolic statement! Go to RADIOLOGY SCHOOL and learn how ionizing radiation works! This is disgraceful!
I think you should educate yourself on radiation exposure in mammography because you are so far from the truth! Also, Please inform me of the false positive/negative results of thermography.
Also, if cancer is found on a thermogram, where do they send the patient to get treated? A breast imaging center?
A mammogram does NOT have the radiation of 1000 chest x-rays! It has only 0.4 mSv. (We naturally receive 3 mSv per year from the environment.) This misinformation could scare some women away from their screening so that they are diagnosed later rather than earlier.
Your sources date as far back as 1977 which makes most of your information outdated and irrelevant in 2019.
As someone who works in Radiology, this entire article is misinforming patients. A chest xray uses a higher technique than a mammogram would. One screening mammogram is less than or equivalent to the amount of radiation recieved from just one chest xray therefore the quote that “You can get as much radiation from one mammogram as you would from 1,000 chest X-rays!” Is completely inaccurate. To compare mammography to Hiroshima is totally false as well and just fear mongering. There is no similarity and the dose equivalents are drastically different.
If your medical doctor thinks this is what is best for you as the patient, then you should listen to your doctor who knows you, your health, and your health risks. Your doctor decided this exam is more beneficial to you than the risk associated with it. Thermography can be a useful tool for someone who is low risk, but no doctor will use this to diagnose or treat. You would still be sent for a mammogram if the thermography test was positive.
A medical doctor, scientist, or researcher did not write this article. This is not from a medical journal with truly accurate sources and information.
Make sure whoever is reading the thermography report knows what they are doing. I did this for years and still had breast cancer, it should have never happened.
Hi there. I live in Johannesburg, South Africa and am looking to see someone here. Would you be able to recommend a Therapist here for this.
Many thanks
Warm regards
Jeannette
This is a horrifically misleading article. Mammograms are in fact a low dose radiation and are certainly not equal to 400 cheat xrays…. not to mention, if you were to fly in an airplane from
Boston to los angeles you would get the same amount of radiation as you would a mammogram. As a mammgrapher, i see the benefits of yearly screenings and these statistics are completly baseless and made up? Comparing mammograms over 10 years to being near hiroshima when the atom
Bomb dropped? You should be ashamed of this article!
I have urvived double mastectomy fukk hysterectomy lung cancer in lobe and lumpectomy left breast after radiation. The found a mass in the left side of my chest under implants again. All cancers have been on left side I hope we have this in Saskatoon Sk Canada . There is hope after all. Thanks for the info will ask my surgeon.
This article is highly disconcerting and probably reaches those people who are more likely to forgo proven screening methods, which is irresponsible and dangerous. Having a mother that died from breast cancer at 38 and then going on to earn degrees in radiation oncology. So many statements in this article are purely false. Not to mention, the logic employed to analyze current studies is grossly flawed. I would like to see you have this peer reviewed by a radiologist or radiation oncologist, make adjustments and then repost. The internet is a great platform, but we should only promote knowledge that is accurate and safe for the audience reading it.
I have had a thermogramme with Dr Nyjon.Eccles in London. fantastic on every level. worth every penny.
I live in N. C. Are their any places here in N. C.??