Excess Calcium Causes Inflammation And This Other Mineral Reverses Inflammation
Last updated on
For the last few decades, people have been taught to take calcium for bones. Drink milk, take calcium supplements for strong bones and teeth. Yet, during the same time, osteoporosis incidences rose at an alarming rate more than ever in history. This might shock you: Excess calcium causes inflammation!
More and more studies are showing that calcium is the main culprit in the cases of most inflammation. Any diseases with names ending with –itis are explaining inflammation of body parts.
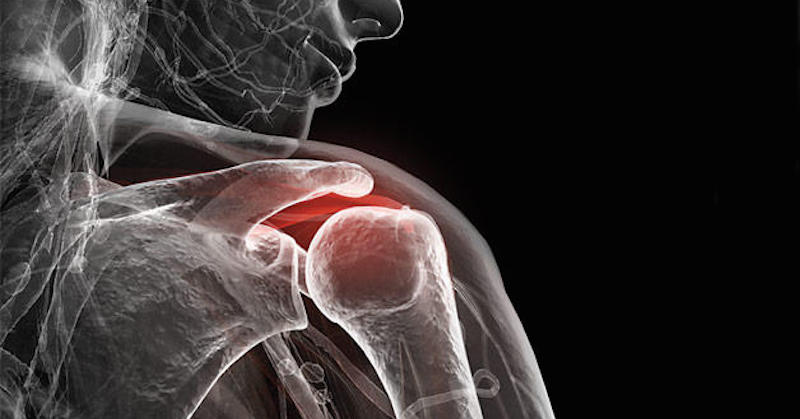
For example, colitis is inflammation of the colon, sinusitis is inflammation of the sinus, bronchitis is inflammation of the bronchi, arthritis is inflammation of the joints (from the word arthrosis), and hepatitis is inflammation of the liver (from the word hepar). You get the idea, they are all the same “disease”, that is inflammation.
Calcium Absorption
A 12-year study tracking about 78,000 nurses found that the more cow’s milk they consumed, the higher the rate of bone fractures were experienced. In countries where dairy and calcium consumption is lowest, bone fracture rates are also the lowest. (Ref: The China Study)
It is not just a matter of taking calcium from foods and supplements for strong bones. There are various important factors that affect whether your calcium intake is properly deposited into the bones, or if they are not absorbed, may cause calcium deposits elsewhere.
Excess Calcium Causes Inflammation
98% of calcium is found in our bones, 1% in our teeth and 1% in other tissues. Calcium that is not deposited in the bones may cause:
- Brittle and fragile bones (osteoporosis)
- Hardening of the arteries (arteriosclerosis)
- Calcification in the brain (intracranial calcification)
- Calcification in the liver and kidneys (liver and kidney stones)
- Calcification in joints (arthritis and gout)
- And many other medical conditions
Factors That Contribute To Calcium Toxicity
Calcium toxicity is a complex issue and it it not simply an overdose of calcium, whether the sources are from food or supplements. Various factors and the nutritional condition of an individual play a part on whether the calcium will be absorbed into the bones, or it will “run loose” in the blood and cause calcification elsewhere.
These are some things to consider:
- Nutrient cofactors—there are many other minerals for healthy bone formation, such as magnesium, boron, manganese, zinc, copper, silicon and phosphorus
- Calcium requires vitamins A, C, D and K for optimal metabolism
High animal protein and dairy consumption may cause an acidic blood that increases calcium loss
- A very high fat intake (of the wrong kinds of fats), and artificial food additives from processed foods inhibit calcium absorption
- Long-term medication and stress deplete the body of various minerals that are necessary for calcium absorption
- Excessive sugar and salt intake deplete the body of minerals that help calcium absorption
- Certain health conditions may also prevent calcium absorption leading to bone loss
- Drinking water that is fortified with “bad” calcium that the body cannot assimilate. Drinking water that contains fluoride also depletes the body of minerals that prevent calcium absorption.
- Taking the wrong kind of calcium supplements
So, is calcium really all that bad? Should you throw out your calcium supplements? The quick and short answer is NO. A quick and short-term solution is to temporarily stop eating excess calcium, and supplement with magnesium to reduce inflammation.
Why Magnesium?
Next to potassium, magnesium is the second most abundant positive-ion-charged element inside human cells. Outside of the cells are calcium and sodium.
Magnesium is a key cofactor in more than 300 enzyme-driven biochemical reactions, and a key mineral in hundreds of functions in the body. The tasks that magnesium is needed in are too complex and sophisticated to be listed in this short article, but you can imagine that the deficiency of this mineral could easily cause all these functions to spiral out of control.
Most of the factors that contribute to calcium toxicity mentioned above, contribute to a depletion and deficiency of magnesium. One of the main functions of magnesium is to absorb calcium and make it available for bone-building. In the absence of magnesium, calcium is malabsorbed and “runs loose” to be deposited elsewhere in the body but the bones. Thus calcification takes place.
Calcium-Magnesium Ratio
In Dr Carolyn Dean’s book, “The Magnesium Miracle”, she explained …
Ideally, the dietary ratio of calcium-magnesium should be 1:1. However, due to magnesium depletion caused by environmental toxins and various other factors, an average diet today has a shocking 10:1 ratio of calcium to magnesium!
The 1:1 ratio should not just be in supplements form, but in the combination of diet, water and supplements. In some cases, people have to take twice the amount of magnesium as calcium to undo the damage from calcium buildup, drug intake, stress and consequent inflammation in the body.
Just as calcium causes inflammation, magnesium is an anti-inflammatory agent that reverses the inflammation.
Magnesium Is Anti-Inflammatory
Magnesium is well absorbed from food sources such as legumes, whole grains, green vegetables, avocados, seeds and nuts (especially almonds). Magnesium is the central element of chlorophyll, the substance that gives plants their green color. So, if it’s a green plant food, consider it as a potentially good magnesium source. See list of foods rich in magnesium and various forms of magnesium supplements.
As each individual is different, your magnesium requirement may be different from another, although you will never get an overdose from magnesium. Your body knows to use only the magnesium you require and excrete any excess.
In her book, Dr Carolyn Dean recommends Natural Calm for magnesium supplement a good place to start if you need help with reducing inflammation in your body.
References:
https://www.greenmedinfo.com/article/higher-consumption-milk-among-women-associated-increased-risk-hip-fracture-45
https://www.ancient-minerals.com/magnesium-benefits/what-is-function/
Some of the links I post on this site are affiliate links. If you go through them to make a purchase, I will earn a small commission (at no additional cost to you). However, note that I’m recommending these products because of their quality and that I have good experience using them, not because of the commission to be made.
Comments
Leave a Reply

 High animal protein and dairy consumption may cause an
High animal protein and dairy consumption may cause an 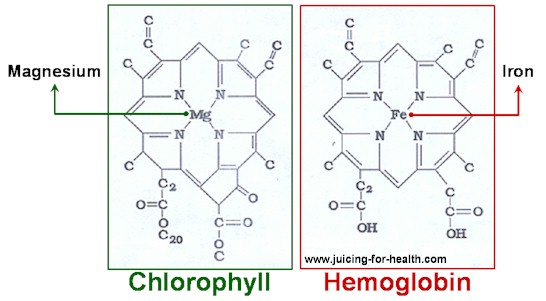































 JOIN OVER
JOIN OVER
Thank you so much. This is a wonderful article. I have loved magnesium for many many years. People need to do their own research and learn how wonderful it is. I grow kale and collards, they are loaded with magnesium and highly absorbing calcium. My hope is that people will study the many many benefits and use it. It works immediately, and I mean within minutes. I use the product CALM magnesium only. I learned that if I stir it in my glass (the small amount I want to take, I start off very small amount) with 16 ounces of water and sip it drinking 1 large gulp every hour, it will nourish my cells and absorb. However if i gulp the glass full it will be like a laxative. Do your research! Some people should not take it like I do. This mineral is a blessing from God.
So much info!!!
I suffer from leg, foot, calf cramps nightly. Have been advised to foot soak (or bath) in magnesium chloride.
Don’t want to take oral as I have controlled hypertension.
Most sites quote Epsom Salts but what is the difference and best to use?
Hi Em, Epsom salt does the job just as well. Add some to a bucket of water and soak your feet every evening. You can also use magnesium oil spray and spray it at the bottom of your feet before you sleep. Here’s a good one: https://amzn.to/2ja6oYR. Take care!